The Extraocular Muscles |
Anatomy, Physiology and |
Ted M. Montgomery, |
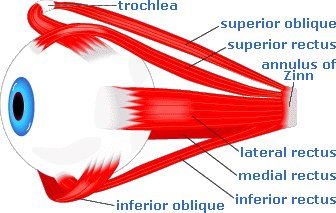
The extraocular, ocular motor or extrinsic eye muscles, considering their relatively small size, are incredibly strong and efficient. There are the six extraocular muscles, which act to turn or rotate an eye about its vertical, horizontal, and antero-posterior axes:
Here is a schematic of a left eye, showing how its extraocular muscles insert into the eye:

Eye muscles work together with other eye muscles, of the same eye and the opposite eye, to move both eyes together in various directions. These are known as yoked eye movements.
However, a given extraocular muscle, if working on its own in isolation and not yoked with other muscles (that is, without other extrinsic eye muscles in play), would move the front of one eye alone in a specific direction or directions, as follows:
The primary muscle that moves an eye in a given direction is known as the “agonist.” A muscle in the same eye that moves the eye in the same direction as the agonist is known as a “synergist,” while a muscle in the same eye that moves the eye in the opposite direction of the agonist is an “antagonist.” According to “Sherrington’s Law,” increased innervation to any agonist muscle is accompanied by a corresponding decrease in innervation to its antagonist
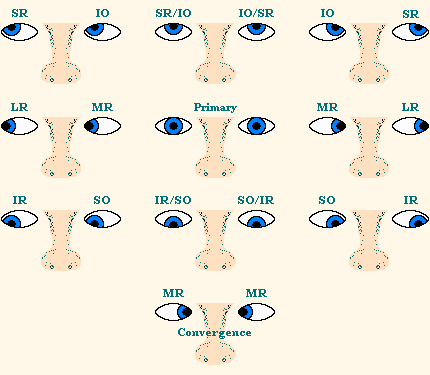
The “cardinal positions” are six positions of gaze which allow comparisons of the horizontal, vertical, and diagonal ocular movements produced by the six extraocular muscles when both eyes and multiple muscles are working together. These are the six cardinal positions:
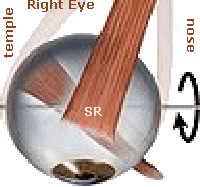 A top view of the right eye is pictured on the left. Notice the right superior rectus (SR) muscle, which inserts at an angle into the top of the eye. Now, imagine the eye being abducted (turned away from the nose) by the lateral rectus (LR) muscle (not pictured). With the right eye looking to the right, if the SR muscle also were to contract, it is not hard to visualize how the front of the eye would move upward.
A top view of the right eye is pictured on the left. Notice the right superior rectus (SR) muscle, which inserts at an angle into the top of the eye. Now, imagine the eye being abducted (turned away from the nose) by the lateral rectus (LR) muscle (not pictured). With the right eye looking to the right, if the SR muscle also were to contract, it is not hard to visualize how the front of the eye would move upward.
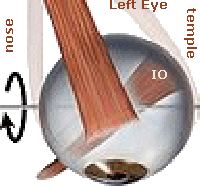 A similar situation is true for the left eye, pictured on the right. The inferior oblique (IO) muscle is seen to insert at an angle into the bottom of the eye. Imagine the eye being adducted (turned toward the nose) by the medial rectus (MR) muscle (not pictured). With the left eye looking to the right, if the IO muscle also were to contract, the front of this eye would move upward as well. Both eyes then would be looking up and to the right.
A similar situation is true for the left eye, pictured on the right. The inferior oblique (IO) muscle is seen to insert at an angle into the bottom of the eye. Imagine the eye being adducted (turned toward the nose) by the medial rectus (MR) muscle (not pictured). With the left eye looking to the right, if the IO muscle also were to contract, the front of this eye would move upward as well. Both eyes then would be looking up and to the right.
This yoked or “conjugate” movement of these two muscles, right SR and left IO, is depicted in the first (top/left) image of the chart above. All of the yoked or conjugate movements of the eyes are shown later in the versions section.
The movement of either eye into an up/right, up/left, down/right, down/left, up, down, right, or left position of gaze involves the linked and associated contractions and relaxations of multiple eye muscles, of the same eye and of the opposite eye, at the same time. The nerve innervations that cause all of this to happen are very complex, but suffice it to say that, normally, all of it happens very smoothly and efficiently.
of the Right SR & Left IO 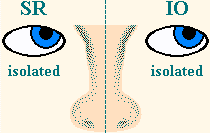 |
Now, look at the graphic of the left eye in the section above. It can be visualized that if the inferior oblique (IO) muscle of the left eye contracts alone, the front of the eye will be pulled upward (supraduction or elevation) and outward (abduction). These and other single muscle movements are not found on the chart in the previous section, as that chart shows only yoked eye movements. The isolated vertical and horizontal movements of all of the extraocular muscles are shown in the muscle movements section.
Each extraocular muscle is innervated by a specific cranial nerve (C.N.):
All of the extraocular muscles, with the exception of the inferior oblique, form a “cone” within the bony orbit. The apex of this cone is located in the posterior aspect of the orbit, while the base of the cone is the attachment of the muscles around the midline of the eye.
The apex of the conic structure is a tendonous ring called the “annulus of Zinn.” Through the annulus, and along the middle of the cone of muscles, runs the optic nerve (cranial nerve II). Within the optic nerve are contained the ophthalmic artery and the ophthalmic vein.
The superior oblique, although part of the cone of muscles, differs from the other muscles in a significant way. Before it attaches to the eye, it passes through a ring-like tendon, the “trochlea,” in the nasal portion of the orbit. The trochlea acts as a pulley for the superior oblique muscle.
The inferior oblique, which is not a member of the cone of muscles originating from annulus of Zinn, arises from the lacrimal fossa in the nasal portion of the bony orbit. This muscle attaches to the inferior portion of the eye.
When considering each eye separately, any movement is called a “duction.” The ductions of each eye are described in the muscle movements section above.
Movement around a vertical axis, “abduction” is a horizontal movement away from the nose, caused by a contraction of the LR muscle, with an equal relaxation of the MR muscle. Conversely, “adduction” is a horizontal movement toward the nose, caused by a contraction of the MR muscle, with an equal relaxation of the LR muscle.
Describing movement around a horizontal axis, “supraduction” (elevation) is a vertical movement upward, caused by the contraction of the SR and IO muscles, with an equal relaxation of the of the IR and SO muscles. Conversely, “infraduction” (depression) is a vertical movement downward, caused by the contraction of the IR and SO muscles, with an equal relaxation of the SR and IO muscles.
Describing movement around an antero-posterior axis, “incycloduction” (intorsion) is a nasal or inward rotation (of the top of the eye), caused by the contraction of the SR and SO muscles, with an equal relaxation of the IR and IO muscles. Conversely, “excycloduction” (extorsion) is a temporal or outward rotation (of the top of the eye), caused by the contraction of the IR and IO muscles, with an equal relaxation of the SR and SO muscles.
When considering how the eyes work together, a “version” or “conjugate” movement involves simultaneous movement of both eyes in a certain direction. Agonist muscles in both eyes, which work together to move the eyes in the same direction, are said to be “yoked” together. According to “Hering’s Law,” yoked muscles receive equal and simultaneous innervation.
There are six principle version movements, where both eyes look or move together, in tandem, in the same direction, simultaneously:
A “vergence,” or “disconjugate” movement, involves simultaneous movement of both eyes in opposite directions. There are two principle vergence movements:
If one eye constantly is turned inward (“crossed-eye”), outward (“wall-eye”), upward, or downward, this is referred as a “strabismus” or “heterotropia,” discussed later.
Usually, a vergence is performed relative to a point of fixation. For instance, someone could be looking at TV across the room (at a far distance). Then, when a commercial comes on, that person could converge both eyes to read a book (at a near distance). Then, after the commercial is over, both eyes would diverge to look at the TV again.
One cannot actually voluntarily diverge both eyes outward, at the same time, from looking straight ahead. That is, the two lateral recti muscles cannot pull the eyes outward, simultaneously and voluntarily, while one is viewing something far away. However, if one is falling asleep with one’s eyes still open, it is possible for the eyes to diverge, momentarily and involuntarily, causing temporary diplopia (double vision).
Normally, when viewing an object, the “lines of sight” of both eyes intersect at the object; that is, both eyes point directly at the object being viewed. An image of the object is focused upon the macula of each eye, and the brain merges the two retinal images into one.
Sometimes, however, due to some type of extraocular muscle imbalance, one eye is not aligned with the other eye, resulting in a “strabismus,” also called a “heterotropia” or simply a “tropia.” Occasionally, this ocular deviation is referred to as a “squint,” although this term is not very descriptive and no longer is commonly used.
With strabismus, while one eye is fixating upon a particular object, the other eye is turned in another direction, relative to the first eye, whether inward (“cross-eyed”), outward (“wall-eyed”), upward, or downward. As a result, the person may experience “diplopia” (double vision), since two different objects are imaged onto the maculas of both eyes. However, if the person’s brain has learned to “suppress” (turn off) the image of the strabismic (turning) eye, the brain will perceive only the single image from the other eye, which typically is the dominant eye.
If the strabismus occurs sometimes, but not all of the time, it is said to be “intermittent.” If the strabismus occurs all of the time, it is said to be “constant.”
Occasionally, whether the strabismus is intermittent or constant, one eye will be the deviating eye at certain times, while the opposite eye will be the deviating eye at other times. That is, one eye will turn sometimes, but at other times the alternate eye will turn. This is referred to as “alternating” strabismus.
The misalignment of a strabismic eye occurs in about 2% of children. The deviant eye may be in any direction: inward (“esotropia” or “crossed-eye”), outward (“exotropia” or “wall-eye”), upward (“hypertropia”), downward (“hypotropia”), or any combination of these.
Strabismus also can occur due to a nerve paralysis or paresis, injury, or even due to a retinal disease. Sometimes a strabismus will result when there is a very different refractive error (usually much higher) in the strabismic eye compared to the other eye.
The angle of deviation of the strabismus is measured in “prism diopters.” If the angle of deviation remains the same in all cardinal positions of gaze, the strabismus is classified as “concomitant” (or “nonparalytic”). If the angle of deviation is not the same in all cardinal positions of gaze, the strabismus is classified as “nonconcomitant” (or “paralytic”).
Below, views of the two most common types of strabismus—esotropia and exotropia—are displayed:
Esotropia can be congenital (a muscle imbalance present from birth), and usually the angle of deviation is large. Management involves surgical correction, typically at age six months or earlier.
Some cases of low-angle esotropia do not require surgery but, instead, respond successfully to visual therapy. This is true especially in a child or an adult for which the esotropia is of recent onset and for which there is no macular damage (that is, when the strabismic eye is capable of good visual acuity).
The esotropia also can be accommodative, usually due to a high amount of uncorrected hyperopia (farsightedness). This causes a great deal of accommodation to be required to focus retinal images, resulting in a subsequent over-convergence (by the medial rectus muscles) and a subsequent esotropia. The usual treatment for accommodative esotropia is eyeglasses or contact lenses, which compensate for the hyperopia, allowing the deviating eye to straighten.
Exotropia also can be congenital, although this is very unusual. More commonly, exotropia develops in infancy or in early childhood, often beginning as an intermittant (occasional) strabismus and sometimes leading to a constant strabismus.
A carefully planned regimen of visual therapy often can be used to treat exotropia, especially in cases where complete suppression of the strabismic eye has not yet occurred and the eye is capable of good visual acuity.
However, in cases where visual therapy is not successful, surgical correction should be used to provide a cosmetically improved appearance of the deviating eye. This does not necessarily ensure that binocular vision will result.
If the vision in a strabismic (deviating or turning) eye is suppressed (turned off) for too long, that eye very well may develop “amblyopia” or a “lazy eye” condition. This means that the visual acuity in that eye no longer is as good as the visual acuity in the other eye, which is used all the time.
In this case, when the normal eye is covered, thus forcing the strabismic eye to take over, the strabismic eye usually does not point exactly straight at the object being fixated. Therefore, the image of the object being viewed does not fall directly upon the macula, as it should. Rather, the image falls upon some eccentric point, away from the macula, where the acuity is not as good. Thus, this is referred to as “eccentric fixation.”
An eye is not a “lazy eye” simply because it turns and does not align with the other eye. Amblyopia (“lazy eye”) simply refers to decreased visual acuity in one eye, compared to the other eye. That is, an eye is referred to as “lazy” because it does not see as clearly as the other eye. The most common reason for amblyopia is the presence of eccentric fixation in a strabismic eye.
Involuntary, rhythmical, repeated oscillations of one or both eyes, in any or all fields of gaze, is nystagmus. It may be pendular (with undulating movements of equal speed, amplitude, and duration, in each direction) or jerky (with slower movements in one direction, followed by a faster return to the original position).
Movements may be horizontal, vertical, oblique, rotary, circular, or any combination of these. Generally, the faster the rate, the smaller the amplitude (and vice versa). The defect is classified according to the position of the eyes when it occurs:
Reduced acuity is caused by the inability to maintain steady fixation. Head-tilting may decrease the nystagmus and is usually involuntary (toward the fast component in jerky nystagmus, or in such a position to minimize pendular nystagmus). Head nodding often accompanies congenital nystagmus. Dizziness or vertigo may be experienced if oscillopsia (illusory movements of objects) occurs.
Nystagmus may be induced with an optokinetic drum or through the stimulation of the semicircular canals. Congenital nystagmus of the pendular type usually accompanies congenital visual impairment (e.g., corneal opacity, cataract, albinism, aniridia, optic atrophy, chorioretinitis). Nystagmus also may accompany a number of neurological disorders, and it may be a reaction to certain drugs (including barbiturates).
There is no known treatment for nystagmus. However, certain types of jerky nystagmus (commonly Grade I types) show spontaneous improvement in childhood (up to about age 10). This type also may be amenable to muscle surgery (essentially, a repositioning of muscles to take advantage of the point of least nystagmus, or position of relative rest).
With the exception of brief experiences of oscillopsia, most individuals with nystagmus perceive objects as being stationary. It is believed that the brain is responsible for the perceptual adjustment.
Educationally, children with nystagmus (who may tend to lose their place in beginning reading instruction) may be helped through the use of a typoscope (card with a rectangular hole, to view one word or line at a time) or an underliner (card or strip of paper to “underline” the line being read). As children with nystagmus mature, they seem to need these support devices less often.
Damage to cranial nerve III, IV, or VI often will cause a “palsy” (paralysis or paresis) of the extraocular
An extraocular palsy may cause the eyes to be misaligned, which is a strabismus. The most common symptom of a muscle palsy is diplopia (double vision)—that is, seeing two images either side-by-side, one on top of the other, or displaced diagonally.
When the oculomotor nerve (cranial nerve III) is damaged, a palsy in the medial rectus, superior rectus, inferior rectus, and/or inferior oblique
In a complete cranial nerve III paralysis, the upper eyelid also will be nearly closed from a ptosis. The pupil might be dilated and unreactive as well.
When the trochlear nerve (cranial nerve IV) is damaged, a palsy of the superior oblique muscle may occur. Typically, this will resut in an excyclotorsion (outward rotation), along with a lesser hypertropia and esotropia (upward and inward movement) of the affected eye. People with this condition will experience both a vertical and a torsional diplopia, and they will compensate for this by tilting the head toward the shoulder of the unaffected eye.
When utilizing the Bielschowsky head-tilt test, the person is told to tilt his/her head toward the shoulder of the affected eye. An overaction of the inferior oblique, and an elevation of the affected eye (and marked diplopia), will result.
When the abducens nerve (cranial nerve VI) is damaged, a palsy of the lateral rectus (LR) muscle may occur, resulting in an esotropia of the affected eye. That eye generally will not be able to look outward past the midline, and it will be somewhat turned inward when the other eye is fixating straight ahead. Diplopia will be observed by the person when he/she gazes to the side with the palsied muscle, and the person will compensate for this by turning his/her face toward the side of the palsied eye.
An extraocular muscle palsy may resolve on its own with time; however, this may not occur. If the palsy and resultant diplopia are permanent, a prismatic correction may be incorporated into spectacle lenses to merge the double images into a single image. Some people prefer simply to keep one eye patched to take away their double vision.
In some cases, muscle surgery is another option. However, it should not be performed for at least six months after the onset of diplopia, since the effects of the palsy may resolve spontaneously over a few weeks or months. If a ptosis (drooping upper eyelid) is involved, such as in a cranial nerve III paralysis, probably the best option is surgical elevation of the eyelid.
The Yoked Extraocular Muscle Movements in Cardinal Positions of Gaze image at this site is used, with permission, in the following article, co-written by Nathan H. Kung, MD, and Gregory P. Van Stavern, MD: Isolated Ocular Motor Nerve Palsies.
Return to the Main Page ![]()
of Anatomy, Physiology & Pathology of the Human Eye
![]()
Copyright © 1998– by Ted M. Montgomery, O.D. Most rights reserved.